Racial bias in health care hurts patients. But that can change.
Menda Stewart had studied symptoms like her daughter had in nursing school. So she took McKenzie to the pediatrician’s office and asked that she be tested for type 1 diabetes. “She doesn’t need that,” the nurse said confidently.

All of a sudden, McKenzie Stewart seemed like an entirely different child.
Usually bubbly and carefree, the 4-year-old was cranky for a solid week. Once proud of her toilet-training progress, she was back to wetting the bed. And she cried constantly about being hungry and thirsty, no matter how much her doting parents gave her to eat and drink.
Her mother, Menda, had studied those symptoms in nursing school. So she took McKenzie to the pediatrician’s office and asked that she be tested for type 1 diabetes.
“She doesn’t need that,” the nurse said confidently.
Stewart firmly but calmly explained her own nursing credentials, and her daughter got the test — and the diagnosis her mother expected.
Stewart, 34, is happy with the care her daughter is receiving. Now 6, McKenzie is thriving. But Stewart suspects things might be different if not for her constant advocacy.
Sometimes, when encountering a new care provider, “I don’t tell them every time I’m a nurse,” she said, “and I think sometimes we get brushed off because we are African American.”
Experts in health-care bias say Stewart’s perception is neither unique nor unfounded.
Families such as the Stewarts must rely on a health-care system that is overwhelmingly white and has historically treated patients of color poorly, even going so far as to use them as subjects of unethical experiments. Lingering distrust and discrimination, research has found, contribute to worse health among minorities, who experience higher rates of heart disease and kidney failure, and a shorter lifespan, on average, than whites.
Even the coronavirus pandemic has disproportionately affected African Americans, who are more vulnerable because they are more likely to have underlying health conditions and who are dying at a greater rate — a disparity U.S. Surgeon General Jerome A. Adams in April attributed to a legacy of “being black in America.” In New Jersey, African Americans account for nearly a quarter of coronavirus deaths for which race data exists, even though they make up just 13% of the state’s population.
Although type 1 diabetes is most common among white children, diagnosis rates are rising fast among black and Hispanic children, according to a national research group that has spent the last 20 years studying the disease among children. The disease is notoriously difficult for any patient and family to manage. But the stakes are particularly high for minority patients.
Consider:
Black and Hispanic children tend to be sicker by the time they are diagnosed, possibly because of clinician reactions like the one Stewart encountered.
Children of color experience more complications and hospitalizations related to the disease than their white peers.
Yet they are less likely than white children to receive medical technology that can improve blood-sugar management, which would help them avoid consequences such as vision loss, kidney failure, poor circulation, and more.
Stewart believes any disadvantage her family may have dealing with exclusively white doctors is countered by her medical training.
“All of McKenzie’s care team is Caucasian, but we don’t have those problems, because I’m McKenzie’s advocate,” Stewart said.
Research shows that providers may not even be aware of race-based attitudes that influence how they perceive patients and the care decisions they make. As more health systems recognize the problem, rooting out “unconscious bias,” as it’s known, is becoming a standard part of medical education.
But attitudes so deeply embedded are slow to change.
“Health care is the canary in the mine. It is an indicator of a sick society,” said Jerry McCauley, chief of nephrology at Jefferson Health, whose decades of work in the field has helped eliminate the racial gap in kidney transplantation. “It’s clear where it’s coming from, and if you know enough about the history, you know how it got that way.”
As deeply entrenched as racism has been, equal quality in health care — such as what McKenzie enjoys — is entirely possible.
Acknowledging and exploring the problem, McCauley notes, is the first step to finding a way out of it.
And through exploring the causes and treatment of type 1 diabetes in minority children, researchers also are chipping away at the mysteries of a disease that could lie not only in our bodies, but also in our history.
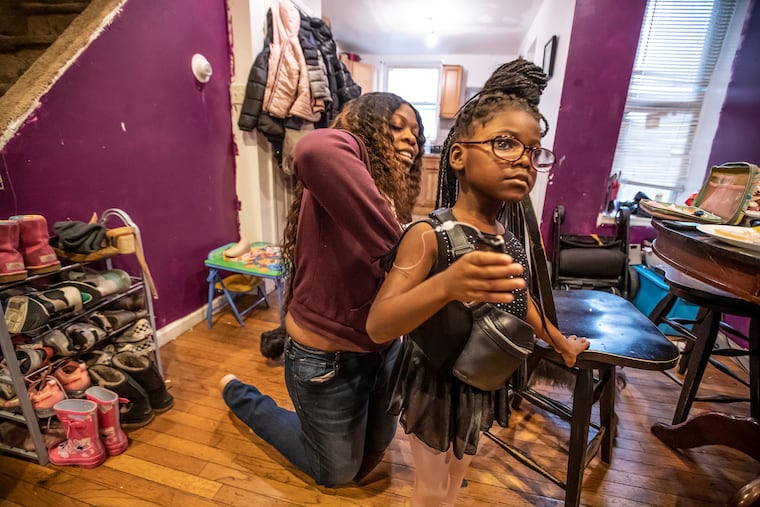

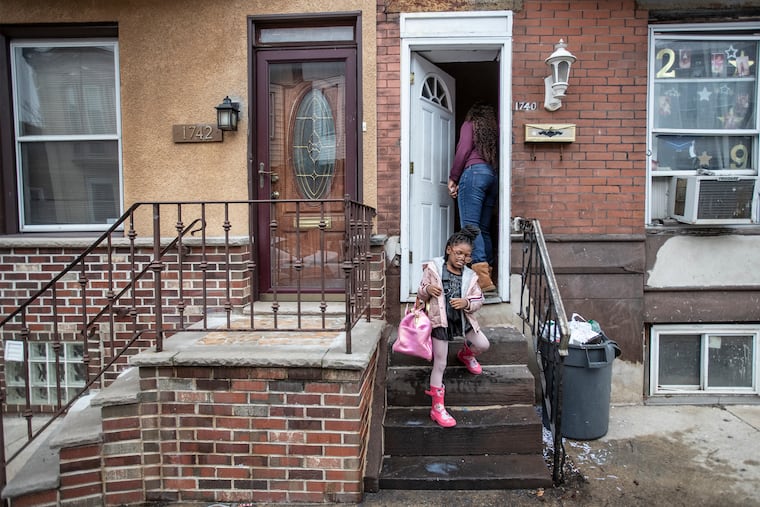
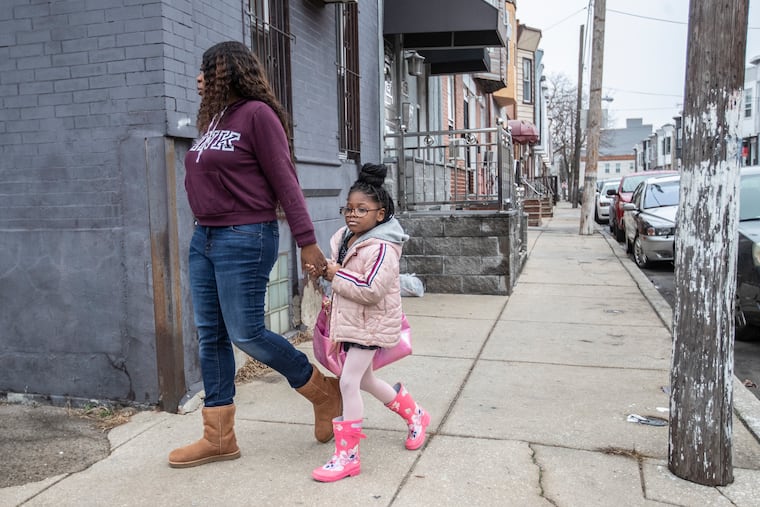






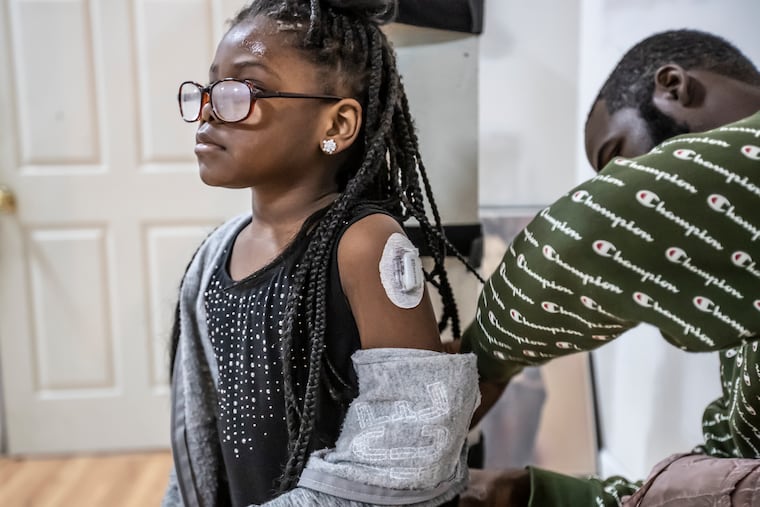



Mystery in the veins
Though income, education, and other socioeconomic factors are associated with racial gaps in health care, those factors alone often don’t explain the disparities. Researchers at the University of North Carolina-Chapel Hill found that money, education, and insurance status make no difference in blood-sugar control among children with type 1 diabetes. Affluent minority families’ children still fared worse than white children.
“No matter how we look at it, we can’t account for the fact that glucose control for kids with type 1 is worse for minority youth than it is for white kids. We can’t explain that,” said Elizabeth Mayer-Davis, chair of the university’s department of nutrition. Her team found that African American and Hispanic children with type 1 were more likely to have high average blood-sugar levels, as well as the greatest short-term increases, compared with white children.
Even more troubling, minority boys and minority children under age 9 had the worst blood-sugar control of all children in the study group, said Anna Kahkoska, a doctoral candidate and the report’s lead author.
“It’s basically the worst case,” she said. Children exposed to higher blood-sugar levels for longer periods of time means “it is reasonable to suspect that complications will likely emerge earlier in life,” Kahkoska said.
Tackling bias
Sicker children need more medical attention. But that can be hard when patients believe that their doctors can’t understand them.
While the American population has become more diverse, nearly two-thirds of all health-care professionals are white, according to data from the U.S. Department of Health and Human Services. Just 16% of health workers are Hispanic and even fewer, just under 12%, are black.
Multiple studies have found that patients are more likely to trust doctors they feel they can relate to. For many, that means providers who look like them and share cultural experiences.
Without a solid provider-patient bond, doctors may believe that they aren’t being understood. Patients may not want to ask questions for fear of being judged or misunderstood.
Managing diabetes has a huge cultural component, given that the entire family’s routines and meals can be affected, further complicating matters.
Stewart, as both a mother and a nurse, has seen such disconnects.
“I speak up, I make sure they do everything they’re supposed to do,” Stewart said. “I definitely feel like McKenzie is at an advantage because I’m a nurse and an advocate for her. I worry about people who don’t have that.”
One example is her 21-year-old cousin in West Philadelphia, who found out she had type 1 diabetes through a phone call from her doctor. The doctor later ordered her a continuous glucose monitor, which automatically tracks blood-sugar levels and can make managing diabetes much easier — if you know how to use it. But the device was delivered in the mail, with no doctor or pharmacist to walk her through its setup.
Six-year-old McKenzie, by contrast, learned from her care team at Children’s Hospital of Philadelphia to make careful glucose control just another part of her busy life. Yes, she has her mother’s constant advocacy. But the family also benefited from a full week at the hospital — standard procedure in Philadelphia when a child is diagnosed with type 1 — full of lessons for both McKenzie and her parents.
On a recent Saturday morning, McKenzie finished ballet class, pranced across the room, and launched into her father’s arms for a quick hug.
With moments to spare before jazz class, she dug into her glitter-encrusted unicorn gym bag and pulled out a zippered kit the size of an iPad containing a monitor and needles, and handed it to her father, Christopher.
As the rest of the girls buzzed around the room, McKenzie sat patiently as he tested her blood sugar. She gobbled down a peanut butter sandwich — she needs to eat a snack and balance her insulin when exercising — rested a beat, then dashed back to her place on the dance floor.
Addressing race-based communication challenges requires doctors to recognize and confront what’s known as implicit bias, beliefs that may be held unknowingly, yet exercise considerable power.
Dan Taylor leads the outpatient pediatrics clinic at St. Christopher’s Hospital for Children. He has devoted his career to caring for his young patients, most of whom hail from the poorest neighborhoods in Philadelphia. He has published widely — including in this newspaper — on how growing up in tough circumstances can set up his young patients for lives of failure unless there are serious interventions to help them plot a better course.
Yet when he took an online bias test offered by Harvard, he was stunned to discover that he viewed white and black patients differently. The test measures how strongly test-takers associate groups of people with various qualities, such as intelligence, athleticism, and goodness. People who quickly connect positive qualities with white and black people equally are considered less biased than those who take longer to make those links.
The realization has changed how he approaches his patients and the Drexel medical students he supervises. But even for a highly motivated physician such as Taylor, it’s not simple.
“It’s a different way of retraining your brain to listen a different way, to pay attention to very subtle expressions or words or emotions that families express,” Taylor said.
And unconscious bias is about even more than that.
Steven Willi, medical director of the diabetes center at CHOP, found that unconscious bias among doctors prescribing insulin pumps likely leads to fewer black children getting the technology, which helps patients keep blood-sugar levels more stable than periodic injections.
In a 2015 study, Willi and his colleagues found that white children from low-income families without private insurance were more likely than black children from wealthier families with private insurance to have this technology.
There are reasons a child may not want an insulin pump: Teenagers may not want to wear a bulky device, while parents may worry about whether the technology is reliable, or whether it’s just another costly gadget.
“Or it may just be you weren’t offered the pump,” Willi said.
“And ‘offered’ can mean a lot of things: ‘Oh, do you think you might be interested? No? OK, that’s fine,’ vs., ‘I really think this is something you should be taking advantage of,’” he said. “In the relationship between the practitioner and the patient, there is a great deal of salesmanship — and implicit bias must influence that.”
Years ago, when the technology was newer and harder to get insurers to cover, there was a sense that patients needed to “earn” a prescription. And implicit bias, Willi believes, played a role in which patients doctors decided were worthy.
“Some kids will do well with the pump, and you can’t always predict it. We thought we could predict it,” he said. “What I learned ... is that everybody has the opportunity to do well. It changed my outlook entirely.”
The Stewarts didn’t wait for someone to offer McKenzie an insulin pump.
After a year of pricking her finger multiple times a day to test her blood sugar, giving her insulin injections, watching everything she ate, and worrying every time she wanted to run around outside in their South Philadelphia neighborhood, Menda told McKenzie’s doctors she wanted her daughter to have an insulin pump.
McKenzie’s doctors agreed and helped her enroll in a clinical trial that would get her an insulin pump and continuous glucose monitor sooner than she would have qualified for them through insurance.
With the pump and CGM, McKenzie is down from as many as eight needles a day to a few a week, to calibrate her devices or test her levels on occasions, such as dance, when she takes them off.
Most important, having the technology gives the Stewarts confidence to let McKenzie be a kid first, and a type 1 patient second.
“It’s very important to me that she feels like the other kids her age,” Stewart said. “Just because you have diabetes doesn’t mean you’re different than anyone else.”
This article was supported by the USC Annenberg Center for Health Journalism 2019 National Fellowship.

